A sneak-peek at the future of employer-sponsored coverage
By Gabrielle Smith on May 5, 2021 at 8:35 AM
New research released by the Kaiser Family Foundation (KFF) reveals large employer’s opinions and concerns about the future of employer-sponsored health coverage.
More than 300 executive decision makers at organizations with over 5,000 employees responded to the survey. Their responses show that the majority (87%) believe the cost of providing health benefits to employees will become unsustainable in the next 5 to 10 years.
KFF reports that the survey highlights a broken healthcare system with uneven quality, bloated costs, and an unsustainable future.
In this article, we’ll break down the KFF survey data, explore potential solutions employers see to the rising costs of healthcare, and introduce a more cost-effective option for employer-sponsored coverage beyond traditional group health insurance.
Learn about cost-effective health benefits options for small employers
What are large employers saying about employer-sponsored health coverage?
The vast majority of large employers surveyed (96%) agree that the high costs of offering healthcare to their employees is excessive, and rightly so. The KFF reports that employer health plans are charged much higher prices for healthcare goods and services than public plans.
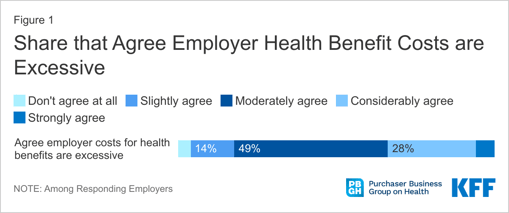
For example, hospitals across the country charge employers and private insurance companies an average of 2.5 times what they get from Medicare for the same care, and three or more times Medicare prices in a half-dozen states.
In addition, the cost of annual premiums for employer-sponsored health insurance have continued to rise. Family premiums reached $21,342 in 2020 (up 55% since 2010) and increased at a rate at least twice that of both wages (27%) and inflation (19%).
Employee deductibles are also experiencing rising prices. Between 2010 and 2020, the average single employee deductible increased from $917 to $1,644 among workers with a deductible.
All of this explains why 87% of the large employers surveyed feel these costs will become unsustainable within the next decade.
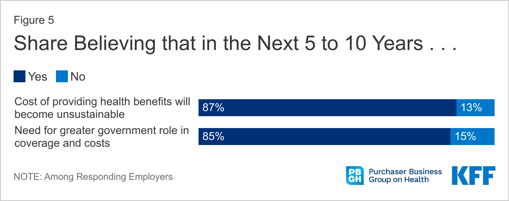
What’s the solution to rising healthcare costs?
The large employers weren’t just surveyed on how they feel about the future of employer-sponsored coverage. They were also asked what solutions they think would best tackle the issue.
The survey results show that most of the large employers found these two solutions to be the most favorable:
- Government action
- Implementing a cost-controlled health benefit
Government action
Many of the large employers surveyed (85%) look to the government to solve the increasing costs of employer-sponsored coverage, both in providing more affordable healthcare and in containing costs in the next 5 to 10 years.
Looking at the numbers, 83% of the large employers surveyed believe that government action will be better for their businesses, while 86% of them believe it will also help their employees.
What’s more, 92% of respondents believe policymakers should pursue policies that would strengthen anti-trust enforcement, as well as prohibit anti-competitive conduct by providers, pharmaceutical manufacturers, and health plans.
When it comes to policies around the transparency of prices and the total cost of healthcare, 90% of respondents said they would support these kinds of actions.
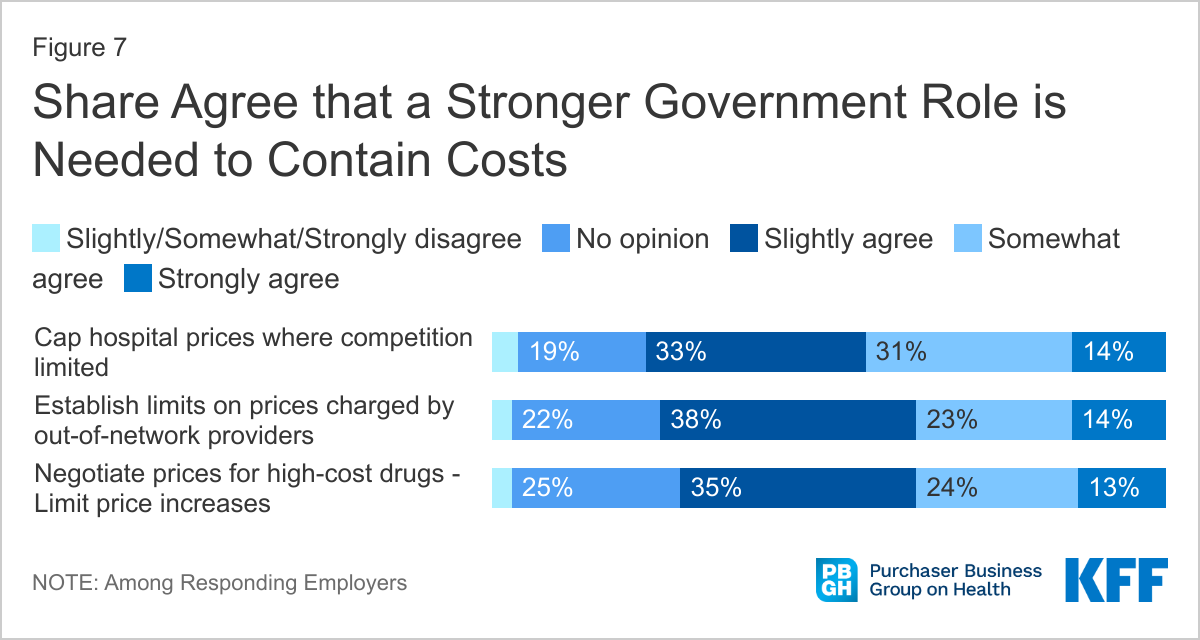
Finally, more than a third of large employers either somewhat or strongly agreed with government policies that would cap prices for hospitals in markets with limited or no competition, limit prices charged by out-of-network providers, and negotiate prices for high-cost, sole-source drugs or set limits on drug price increases.
Implementing a cost-controlled health benefit
Another solution the large employers surveyed favored was transitioning away from traditional group health insurance plans to a more cost-effective form of employer-sponsored coverage. One of these more cost-controlled options is health reimbursement arrangements (HRAs).
Through an HRA, employers provide a monthly allowance to their employees to spend on their own individual health insurance plans as well as over 200 qualifying out-of-pocket medical expenses.
By offering an HRA, you set the budget, giving you complete control over the cost year-to-year, with no annual rate hikes or spiking insurance premiums to worry about. In addition, you’ll only pay employees for the expenses they incur in the plan year, so any unused allowance at the end of the year goes back to you.
Specifically for the employers surveyed, 88% of them reported either being moderately or highly likely to implement an individual coverage HRA (ICHRA) to offer alternative coverage to their employees.
An ICHRA can be used by organizations of all sizes, and employers can choose who participates in the benefit based on employee classes that you determine, including part-time, full-time, seasonal, or salaried workers.
New to ICHRAs? Get everything you need to know in our comprehensive guide
Conclusion
With rising premium costs, overpriced hospital charges, and a lack of transparency on the true cost of healthcare, the future of employer-sponsored coverage can seem daunting. However, with formal health benefits options like HRAs, employers can feel empowered to offer their employees a quality health benefit without the big sticker prices.
PeopleKeep’s benefits automation software and award-winning customer support team helps thousands of organizations administer their own HRAs everyday. See how we can help you control the cost of your healthcare benefits today.
Check out more resources
See these related articles

10 Questions to Ask about Employee Contribution Strategies
Employers use employee contribution strategies to control costs. Ten questions to ask about employee contribution strategies.

Can an employer contribute different amounts toward health insurance?
Can an employer contribute different amounts towards employee medical insurance? Learn the rules for using employee classes to customize benefits.

Pros and cons of stand-alone HRAs
Stand-alone HRAs can offer flexibility and control over healthcare expenses, allowing employers to customize plans to meet their employees' needs.


